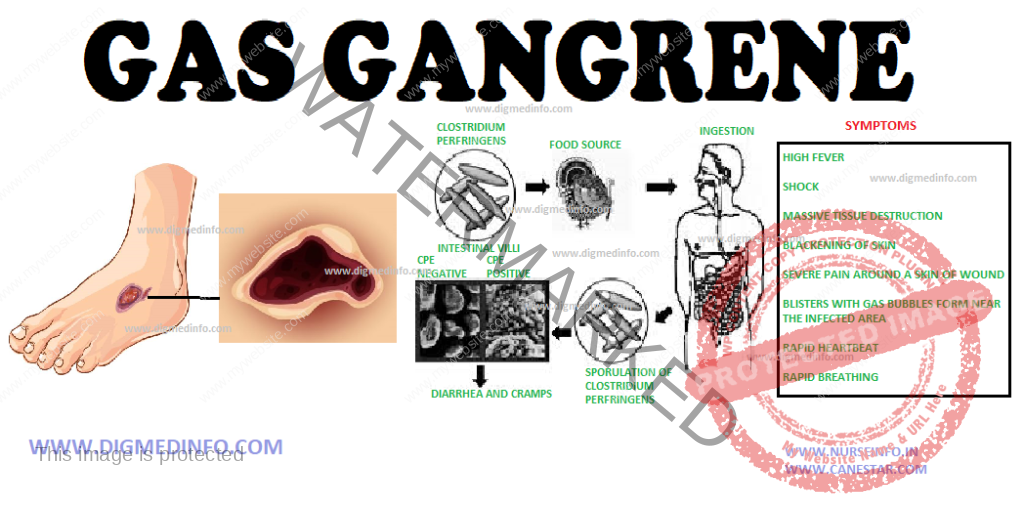
GAS GANGRENE (Clostridial myonecrosis – General Characteristics, Pathogenesis, Clinical Features, Diagnosis and Treatment
General Characteristics
Gas gangrene is caused by Clostridium perfringens (C.welchii), C. septicum, C. novyi (C. oedematiens) C.histolyticum and C. sordelli. These clostridia are commensals in human gut and soil. They produce local necrosis and distant lethal effects.
Pathogenesis
Necrosis of tissue brought about by anoxia, ischemia or injury is complicated by clostridial infection which may be exogenous (introduced along with the wounds) or endogenous (derived from the intestinal tract). The organisms multiply locally and produce toxins which diffuse out and lead to generalized toxemia. The affected tissues are avascular and appear as if cooked.
Clinical Features
After an incubation period of 1-4 days the wound becomes swollen and tender and exudes brownish foul-smelling fluid. Due to the presence of gas, crepitus may be felt. Blebs filled with purplish foul-smelling fluid develop. These blebs rupture and ulcerate. General symptoms such as restlessness and fever develop and the patient may rapidly go into shock and anuria.
Diagnosis
The condition has to be diagnosed clinically. The organism can be identified by culture. X-ray of the affected part shows gas in the tissues. Gas in the tissues may occur in other conditions such as surgical emphysema and infections by streptococci, staphylococci and E. coli.
Treatment
Early institution of therapy is most important for success. Shock is treated on the lines of septic shock. Penicillin which is the drug of choice is given intravenously in a dose of 2 mega units 2 hourly. Other antibiotics may be tried depending on the sensitivity tests. Metronidazole and gentamicin are effective in most cases. Antitoxin is available for intravenous use (anti-gas gangrene serum—AGGS). It should be given in a dose of 40,000 units initially to be followed by 20,000 to 40,000 units repeatedly till the condition improves. Keeping the patient under hyperbaric oxygen (3 atmosphere pressure) remarkably improves the result of therapy and this should be instituted wherever it is available. Surgical excision of dead tissue and removal of foreign bodies should be undertaken after administration of AGGS. Gas gangrene can be prevented by taking proper care of the wound and early recognition of the condition.