PELLAGRA – General Features, Pathology, Clinical Features, Skin Changes, Course and Prognosis, Treatment and Prevention
General Features
This disease was widely prevalent in India among the maize eating communities in all states, especially Andhra Pradesh, Tamil Nadu and Rajasthan. Consumption of sorghum or jowar also predisposes to this tendency. Newer varieties of maize and sorghum with better nutritive value have helped to reduce the incidence of pellagra.
Alcoholism and malabsorption states precipitate pellagra. Inborn disorders of metabolism such as Hartnup disease in which the absorption of tryptophan is impaired lead to pellagra in rare cases.
Pathology
Dermatitis, changes in the oral and intestinal mucosa and degenerative changes in the central nervous system are seen. Ulcers may develop in the intestines. Chromatolysis of ganglion cells occurs in the central nervous system. Patchy demyelination occurs in the spinal cord.
Clinical features
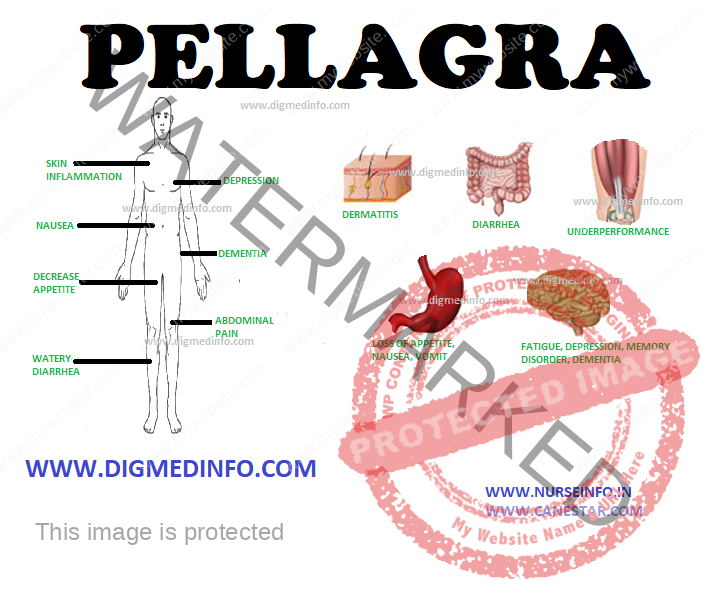
Generalized malnutrition is evident in most cases. The most well-known features are the three Ds—dermatitis, diarrhea and dementia, but these characterize the very advanced stage of the disease. Pellagra should be diagnosed much before this classical picture develops, since the advanced stage is associated with high mortality.
Skin changes
These are seen over areas exposed to sunlight. These start with erythema which may resemble sunburn. This progresses to vesiculation, ulceration, secondary infection, and crusting. In chronic pellagra the skin becomes rough, thickened, scaly and pigmented. In
home-bound patients not exposed to the sun, pellagra may develop without the skin changes—“Pellagra sine pellagra”.
Mucous membrane changes are evident in the mouth and vulva. Skin of the perianal region shows degenerative and inflammatory lesions. The tongue is raw and beefy in appearance. Angulostomatitis may be present.
Alimentary symptoms
Vague alimentary symptoms like anorexia, nausea, vomiting, and dyspepsia are invariably seen. Diarrhea is common but not always present. The stools may be watery or rarely dysenteric.
Neurological features
Anxiety, depression, irritability and failure to concentrate are early symptoms. Advanced cases show delirium, dementia and psychiatric manifestation. Mental symptoms may be mistaken for primary psychiatric disorders.
Course and prognosis
Advanced cases are fatal due to diarrhea, secondary infections, or other associated nutritional disorders. Early treatment reverses the symptoms completely.
Treatment
Well-balanced diet containing adequate supply of proteins should be instituted. Nicotinamide is well absorbed if given orally. It is given in a dose of 100 mg every 6 h for 2-3 weeks. In the advanced cases 50-100 mg may be given intramuscularly or intravenously.
Supplements such as the other B complex vitamins and iron should be concurrently administered. Local application of antihistamine creams and protective clothing gives relief to the skin lesions.
Prevention
In maize eating communities other sources of niacin should be provided along with. In non-endemic areas pellagra may develop in the elderly, inmates of mental homes, etc. Such groups require vitamin supplementation.