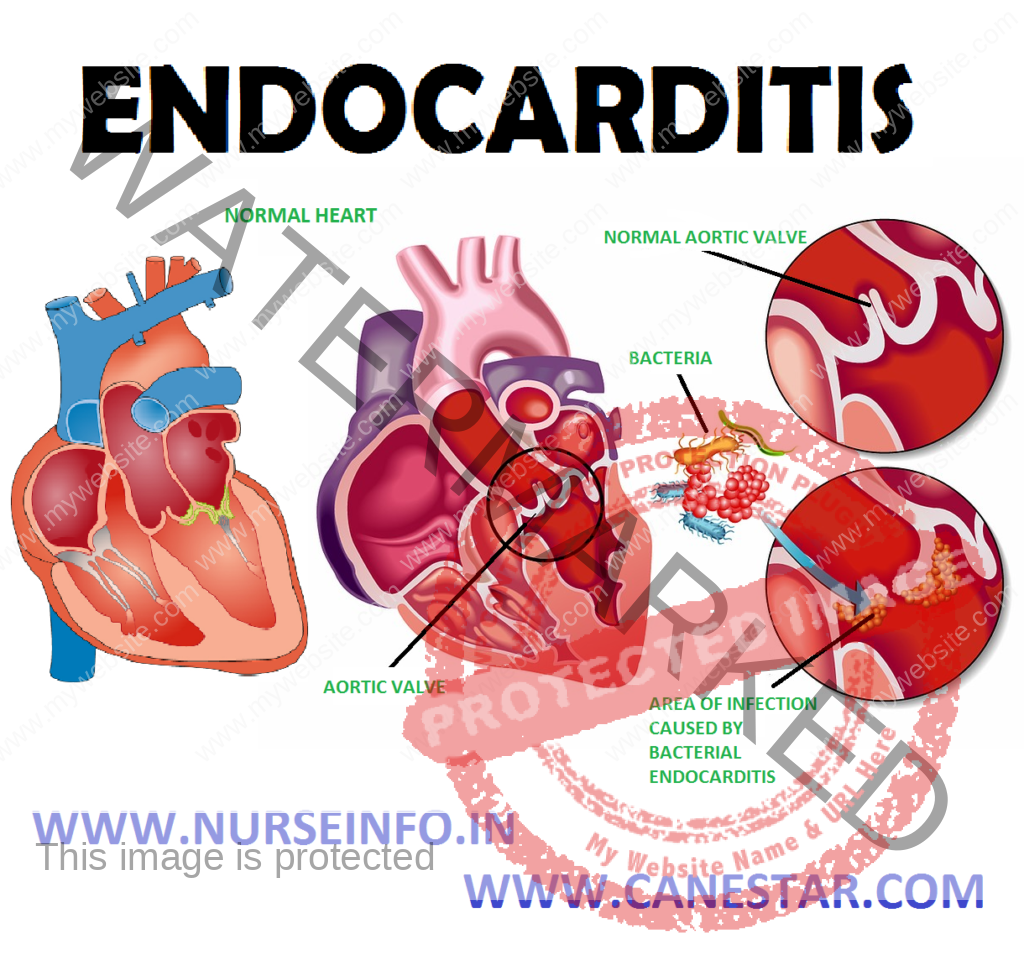
ENDOCARDITIS – Etiology, Risk Factors, Pathophysiology, Signs and Symptoms, Diagnostic Evaluation and Management
Endocarditis is an infection of the heart’s valves or its inner lining (endocardium). It is most common in people who have a damaged, diseased, or artificial heart valve, caused by bacterial infection.
ETIOLOGY
Endocarditis is caused by bacteria that enter the bloodstream and settle on the inside of the heart, usually on the heart valves. Bacteria can invade in the bloodstream in the many ways, including during some dental and surgical procedures. If one does not take care of teeth, then chances of endocarditis increase. Streptococcus viridians is responsible for about 50% of all bacterial endocarditis cases. This is why dental procedures increase chances for developing this condition. Other common agents include staphylococcus aureus and Enterococcus. Staphylococcus aureus can infect normal heart valves and is the most common cause of infectious endocarditis in intravenous drug users.
RISK FACTORS
- Had endocarditis in the past
- Hemodialysis for kidney failure
- Abnormal or damaged heart valves
- An artificial heart valve
- A congenital heart defect
- Hypertrophic cardiomyopathy
- Injected illegal drugs using dirty needles or without cleaning the skin
- HIV
- Coronary artery bypass graft surgery (bypass surgery)
- Previous rheumatic fever without heart valve damage
- A pacemaker or an implantable cardioverter-defibrillator (ICD)
- A heart attack without other complications
- Mitral valve prolapse without mitral valve regurgitation or unusually thickened valve leaflets
- A coronary artery stent
PATHOPHYSIOLOGY
Entry of microorganism in the bloodstream —- colonization occurs on endothelium —- replication of microbes occur —- platelets and fibrins surround the microbes —- bacteria stimulate the humoral immune system —- nonspecific antibodies are produced —- microbes become less vulnerable to antibodies due to platelets and fibrin coverings
SIGNS AND SYMPTOMS
- Chills and fever
- Fatigue
- Weight loss
- Night sweats
- Painful joints
- Persistent cough and shortness of breath
- Bleeding under the fingernails
- Tiny purple and red spots under the skin
- Nail abnormalities (splinter hemorrhages under the nails)
- Night sweats (may be severe)
- Paleness
- Red, painless skin spots on the palms and soles (Janeway lesions)
- Red, painful nodes (Osler’s nodes) in the pads of the fingers and toes
DIAGNOSTIC EVALUATION
A physical examination may reveal:
- Enlarged spleen
- Splinter hemorrhages in the fingernails
- A history of congenital heart disease raises the level of suspicion. An eye examination may show bleeding in the retina a central area of clearing. This is known as Roth’s spots
The following tests may be performed:
- Blood culture and sensitivity (to detect bacteria)
- Chest X-ray
- Complete blood count (may show mild anemia)
- CT scan of the chest
- Echocardiogram (ultrasound of the heart)
- Erythrocyte sedimentation rate (ESR)
- Transesophageal echocardiogram
MANAGEMENT
The American Heart Association recommends preventive antibiotics for people at risk for infectious endocarditis before:
- Certain dental procedures
- Surgeries on respiratory tract or infected skin, skin structures, or musculoskeletal tissue
Antibiotics are more likely to be recommended to those with the following risk factors:
- Artificial heart valves
- Certain congenital heart defects, both before or possibly after repair
- History of infective endocarditis
- Valve problems after a heart transplant
NURSING MANAGEMENT
Nursing Diagnosis
- Hyperthermia related to infection of cardiac tissue as evidenced by temperature elevation, diaphoresis, chills, malaise, tachycardia and tachypnea
Intervention
- Monitor temperature as appropriate to determine effectiveness of therapy and to prevent treatment-induced hypothermia
- Administer antipyretic medication as appropriate or as ordered to reduce fever
- Administer medications as appropriate to treat the cause of the fever
- Monitor white blood cell count to evaluate a patient’s response to treatment
- Monitor vital signs to assess cardiorespiratory response to fever
- Encourage intake of oral fluids to replace fluids lost as a result of fever
- Activity intolerance related to generalized weakness, arthralgia, and alternation in oxygen transport secondary to valvular dysfunction
Intervention
- Monitor cardiorespiratory response to activity (e.g. vital signs) to plan or alter activities
- Monitor patient for evidence of excess physical (e.g. tachycardia, hypertension, diaphoresis, dyspnea) or emotional fatigue to plan for changes in activity level
- Instruct patient/caregiver to recognize signs and symptoms of fatigue that require reduction in activity (e.g. pulse increases> 20 beats/min; no increase in activity if resting pulse > 100 beats/min) since these signs indicate excessive cardiac effort
- Encourage alternate rest and activity periods to reduce cardiac workload
- Deficient knowledge related to lack of experience and exposure to information about disease and treatment process
- Review patient’s and caregiver’s knowledge about condition to identify teaching needs
- Discuss common signs and symptoms of the disease (e.g. fatigue, malaise, chills, elevated temperature, anorexia) so health care provider can be notified and treatment initiated promptly
- Discuss lifestyle changes that may be required to prevent future complications and/or control the disease process (e.g. avoiding persons with infection, taking prophylactic antibiotics before dental procedures) to reduce the risk of recurrent infective endocarditis
- Teaching: prescribed medication
- Provide the patient and caregiver with information about the action, purpose and side effects of the medications to promote safe medication therapy