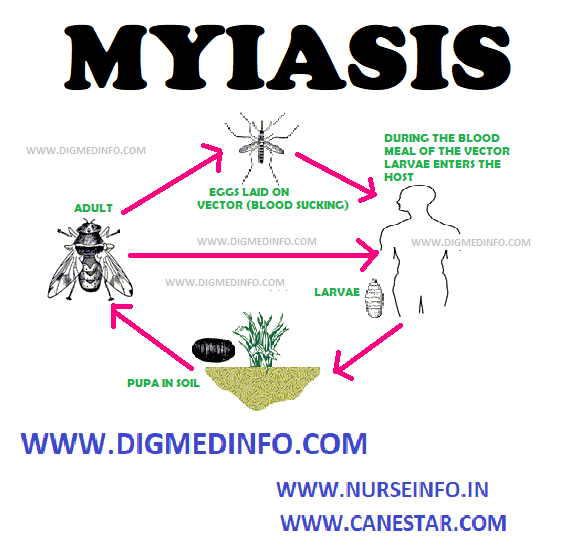
MYIASIS – General Characteristics, Classification, Cutaneous Myiasis (localized), Deep Myiasis, Ophthalmic Myiasis, Intestinal and Urinary Myiasis
GENERAL CHARACTERISTICS
Invasion of tissues or body cavities by the larvae (maggots) of dipterous flies is called myiasis. Myiasis may be of either primary or secondary type. In primary myiasis the human infection occurs as part of the obligate life-cycle of the parasite and in secondary myiasis the human infection is accidental. Primary myiasis affects persons in good general health, whereas secondary myiasis supervenes on dead or necrotic tissues.
Classification:
In general, the infection is of two types:
1. Ectoparasitic, Auchmeromyia leuteola,
2. Endoparasitic.
a. Cutaneous, e.g., caused by Dermatobia hominis and Cordylobia anthropophaga,
b. Tissues or cavities, e.g., caused by Sarcophaga, Wohlfartia, Fannia, Oestrus, Chrysomia, and Callitroga.
The maggots are dull white or pink in colour, actively motile and have spines on their body. The body is tapered and segmented, the narrow anterior end bears the mouth parts, the thicker posterior end bears the opening of the spiracles which are dark coloured and useful in identifying the genera. Their length varies from 0.5 to 3 cm. The larvae feed voraciously on tissues or discharges and in 2 to 4 weeks develop and fall off to the ground to pupate.
Final identification of the species can be done by allowing the larvae to complete the life-cycle in vitro and examining the adult flies.
CUTANEOUS MYIASIS – ECTOPARASITIC
Auchmeromyia leuteola (Congo maggot fly) This fly lays eggs on soil and crevices in the floor. The larvae hatch out in 2 days. They can survive drying and starvation upto one month. Once hatched out, they attach themselves to the skin of the humans who sleep on the floor unprotected, suck blood for 20 minutes and drop off leaving maculopapular lesions. This process is repeated several times before the larva pupates in 2-12 weeks. Bites can be prevented by protective clothing or insect repellents like dimethylphthalate or N-N diethyl benzamide.
Localised Cutaneous Myiasis
Dermatobia hominis (Human bot fly or warble fly) The adult fly lays eggs on hematophagous insects like mosquitoes, stomoxys and ticks or others such as housefly (Musca). When the latter alights on man, the larvae hatch out and wriggle on to the surface. They enter through the wound, produced by the insect or penetrate the unbroken skin and develop in the subcutaneous tissues.
The initial lesion is papular and pruritic. It becomes furuncle-like and painful later. The posterior end of the actively motile larva may be seen in the lesion through the opening. In 2-3 months the larvae mature and fall off to the ground. Lesions are seen on the exposed parts. The disease is worldwide in distribution.
Cordylobia anthropophaga (African tumbu fly) The adults lay eggs on clothes spread out for drying or in dirty soil.
The larvae develop in 24-48 hours and penetrate the human skin either from the clothes or through the bare feet.
The lesion is initially papular and pruritic and becomes painful in a short time. Secondary infection may occur. Unlike the former, the life-cycle is shorter and is completed in 2-3 weeks.
Treatment
The maggots may be extracted surgically. A drop of mineral oil placed on the lesions suffocates the larvae which wriggle out and can be extricated. Penicillin in usual doses should be used to prevent secondary infection.
Migrating lesions resembling cutaneous larva migrans are produced by the larvae of genus Gastrophilus (horse bot flies) and Hypoderma (cattle bot flies), which develop from eggs laid on the hairs. Man is an accidental host and the larvae penetrate the skin, enter the subcutaneous tissues and wander producing eruptions similar to larva migrans of Ancylostoma braziliense, but more painful. They survive for a few weeks and die. Application of mineral oil over the lesions helps to visualize the underlying larvae. Tissues of the eye may be affected. In addition to surgical removal, symptomatic relief may be obtained by antihistamines.
DEEP TISSUE MYIASIS
Larvae of the flies belonging to the families Callitroga (Cochliomyia), Chrysomyia, Sarcophaga, Wohlfartia, Fannia and Oestrus invade tissues extensively when the eggs are laid on open wounds, damaged tissues or discharging surfaces, by the adult flies. The larvae of Wohlfartia can penetrate even unbroken skin.
The lesions are commonly seen in the nasal cavities, paranasal sinuses, middle ear and orbit. Cartilage and bone may also be destroyed by the screw-shaped larvae which may extend intracranially leading to fatal meningitis. The lesions are very painful and the larvae may be discharged from these sites.
TREATMENT
Treatment is manual removal of larvae or extraction after spraying the area with chloroform. Repeated sessions may be necessary.
Secondary infection has to be treated with broad spectrum antibiotics like ampicillin.
OPHTHALMIC MYIASIS
Flies of the genus Chrysomyia and Oestrus may lay their eggs in the conjunctival sac. The larvae hatch out and produce lesions resembling acute conjunctivitis with severe irritation. Rarely corneal ulceration and loss of sight may occur.
Removal of the maggot after anesthetising the eye and application of topical antibiotic drops will relieve the condition.
INTESTINAL MYIASIS
The larvae or pupae of Musca, Fannia, Sarcophaga and Tubifera may be passed in stools or appear in vomitus. The eggs may be laid by the flies around the lips or anus while sleeping, especially if there foul smell discharges around these orifices.
The larvae hatch out from a few hours to two days and are swallowed to reach the upper gastrointestinal tract or they may crawl up into the rectum and large intestine.
They develop in the stomach or in the intestines. Sometimes larvae may be swallowed along with infested foodstuffs. The larvae cause symptoms of gastritis or colitis which may persist from weeks to months. If reinfection does not occur, the condition is self-limiting. Treatment consists of administration of purgatives and reassurance about the self-limiting nature of the illness.
URINARY MYIASIS
Larvae of Muscae, Fannia or Sarcophaga may enter the bladder, when the eggs are laid around the external genitalia and produce symptoms of lower urinary tract infection with proteinuria, pyuria and hematuria. The larvae may pass in urine. Rarely urinary system may be involved by maggots eroding their way from the gastrointestinal tract.