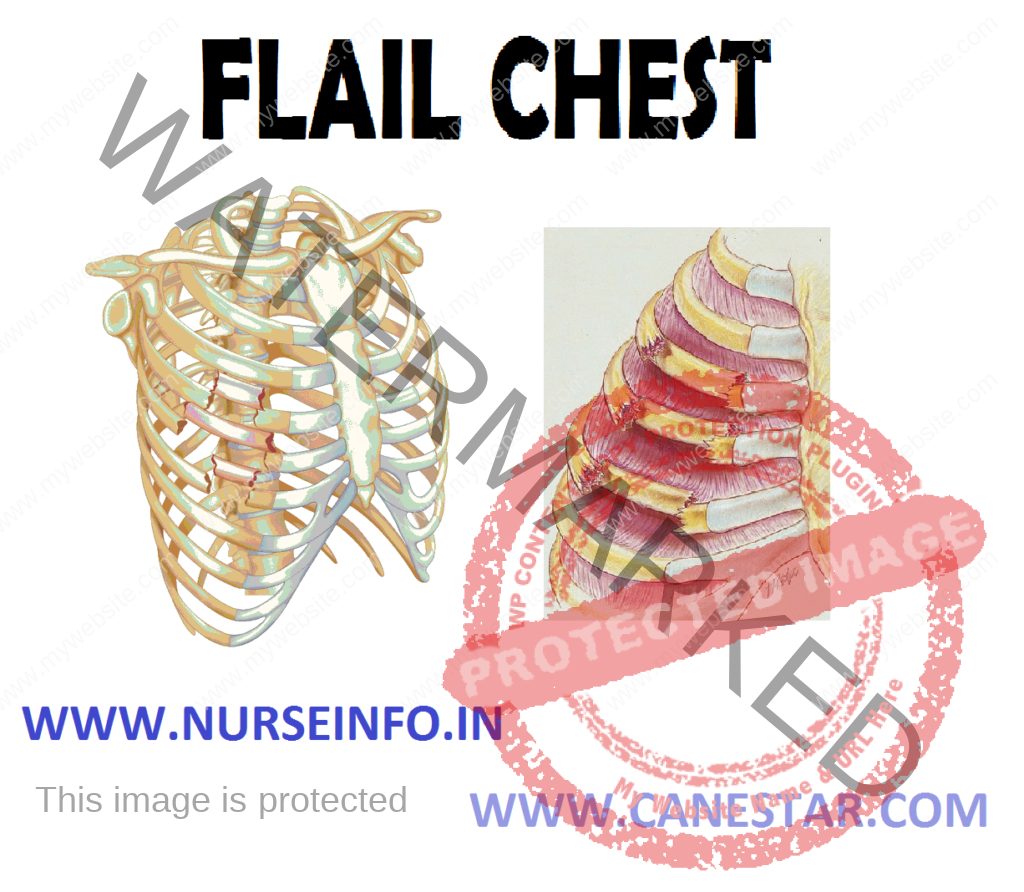
FLAIL CHEST – Characteristics, Etiology, Signs and Symptoms and Treatment
A flail chest is a life-threatening medical condition that occurs when a segment of the rib cage breaks under extreme stress and becomes detached from the rest of the chest wall. It occurs when multiple adjacent ribs are broken in multiple places, separating a segment, so a part of the chest wall moves independently.
CHARACTERISTICS
- During normal respiration, the diaphragm contracts and intercostals muscles push the rib cage out. Pressure in the thorax decreases below the atmospheric pressure, and air rushes in through the trachea. However, a flail segment will not resist the decreased pressure and will appear to push in while the rest of the rib cage expands.
- During normal expiration, the diaphragm and intercostals muscles relax, allowing the abdominal organs to push air upwards and out of the thorax. However, a flail segment will also be pushed out while the rest of the rib cage contracts
ETIOLOGY
This typically occurs when three or more adjacent ribs are fractured in two or more places, allowing that segment of the thoracic wall to displace and move independently of the rest of the chest wall. Flail chest can also occur when ribs are fractured proximally in conjunction with disarticulation of costal cartilages distally. For the condition to occur, generally there must be a significant force applied over a large surface of the thorax to create the multiple anterior and posterior rib fractures. Rollover and crushing injuries most commonly break ribs at only one point – for flail chest to occur, a significant impact is required, breaking the ribs in two or more places.
SIGNS AND SYMPTOMS
- Fracture is extremely painful, and untreated, the sharp broken edges of the ribs
- Puncture in the pleural sac and lung
- Pneumothorax
TREATMENT
Treatment of the flail chest initially follows the principles of advanced trauma life support. Further treatment includes:
- Good analgesia including intercostals blocks, avoiding narcotic analgesics as much as possible. This allows much better ventilation, with improved tidal volume, and increased blood oxygenation
- Positive pressure ventilation, meticulously adjusting the ventilator settings to avoid pulmonary barotrauma
- Chest tubes as required
- Adjustment of position to make the patient most comfortable and provide relief of pain
- Aggressive pulmonary toilet
SURGICAL FIXATION
- Can help in significantly reducing the duration of ventilator support and in conserving the pulmonary function
- A patient may be intubated with a double lumen tracheal tube. In a double lumen endotracheal tube, each lumen may be connected to a different ventilator. Usually one side of the chest is affected more than the other. So each lung may require drastically different pressures and flows to adequately ventilate